The risk of cardiac-induced sudden death peaks in the general population from 6:00 AM to 12:00 noon,1 but in people with obstructive sleep apnea (OSA), the peak in cardiac-induced sudden death occurs during sleep.2 OSA is characterized by recurrent upper airway collapse associated with arousal and/or oxygen desaturation. Although most of OSA is a chronic illness, some patients may be in particularly critical condition due to acute cardiopulmonary failure.3 In this report, we describe a patient with OSA who experienced unexpected critical oxygen desaturation during diagnostic polysomnography.
Case Report
A 53-year-old man was evaluated by the emergency department for dysarthria and lethargy. He was fully conscious and showed no focal neurologic sign, except slurred speech and mild gait instability. He underwent brain magnetic resonance imaging with angiography to exclude acute stroke, but no abnormalities were detected. Several hours later, after the patient was hydrated, the dysarthria and a gait instability improved, but he continued to be lethargic and fatigued. On further interview, he had no specific medical history except a long history of habitual snoring, witnessed apnea, and nocturia. Body mass index was 23.4 kg/m2. He was a current smoker of 60 pack-years. He denied the any use of drugs or hypnotics, but reported alcohol consumption. The patient usually consumed alcohol twice weekly; however he reported recent stress and consumed two bottles of Soju (Korean wine) everyday for 4 days (19% alcohol per 360 mL bottle).
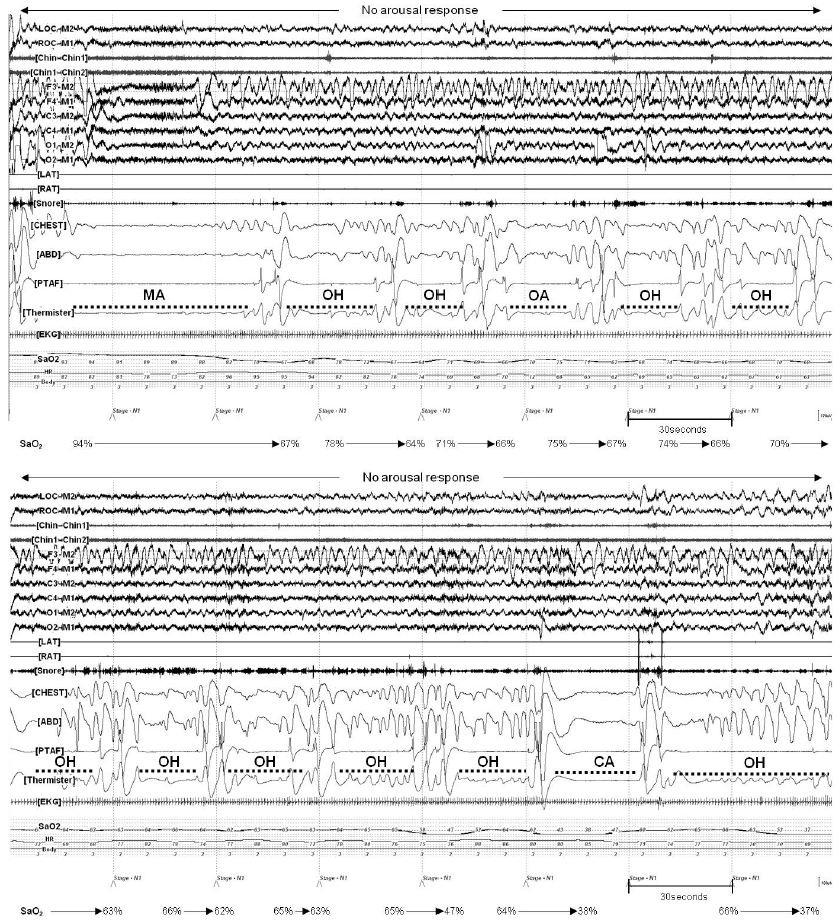
One day after admission, a polysomnography was performed and documented severe OSA, with an apnea-hypopnea index of 44.7. There were recurrent obstructive hypopnea or apnea lasting 15 to 100 s, and the oxygen saturation showed a stepwise decrease (94% to 67%, 71% to 67%, 66% to 62%, and 65% to 47%) over 5 hours since the beginning of the study (Fig. 1). The oxygen desaturation was not accompanied by any electrocardiographic abnormality, though a shortened R-R interval was observed. The electroencephalography did not show any arousal response. The sleep technician shook the patient to awake him, but the patient remained poorly responsiveness for approximately one minute. The patient appeared to be in a state of deep sleep. Finally, he woke up and recovered alert consciousness, and the respiratory event was terminated. We prescribed continuous positive airway pressure (CPAP) with 8 cmH2O after CPAP titration but the patient was not compliant. We lost follow-up after discharge.
Discussion
Obstructive sleep apnea is characterized by repeated cycles of upper airway obstruction, hypopnea or apnea, and arousal.4 This cause repetitive intermittent hypoxemia and sympathetic activation, with numerous deleterious consequences, including adverse cardiopulmonary interactions, endothelial dysfunction, inflammation, and impaired glucose metabolism.5 These multiple phenomena may cause sudden death in OSA patients. OSA is strongly associated with arrhythmias including malignant ventricular rhythms, which may also cause sudden death. Other etiologies inciting sudden death include extreme hypoxemia, particularly in morbidly obese patients, and an absent homeostatic response to pharyngeal closure.
Upper airway obstruction is resolved by arousal or arousal-independent reflexive upper airway opening. However, numerous conditions can affect this reflex or increase the arousal threshold such as acute sleep deprivation, sedatives, narcotics, and systemic illness, resulting in sudden death.3 Notably, our patient was exhausted by stress and heavy alcohol consumption, conditions that can increase the arousal threshold and lead to exaggerate upper airway obstruction. Finally, these conditions might have provoked a critical oxygen desaturation in this patient.
Physicians should consider OSA in cases of patients with sudden cardiopulmonary failure during sleep, particularly those who have no specific medical history. Untreated OSA can cause cardiopulmonary failure, and patients who have recovered from these events need to be evaluated for sleep disordered breathing. Moreover, sedatives and analgesics should be used carefully in patients with OSA.