Obstructive sleep apnea (OSA) is a sleep-concerned breathing disorder that involves a decrease or complete stop in airflow in spite of an ongoing effort to breathe [1]. OSA is an independent risk factor for metabolic disorders such as hypertension and diabetes mellitus, as well as cardiovascular and cerebrovascular disease. For these reasons, it is a disorder that should be properly treated.
Continuous positive airway pressure (CPAP) therapy is a highly effective treatment for the patients with OSA. However, CPAP adherence, how well the patients use it, is a limiting factor to determine the effectiveness on OSA treatment [2]. There are several ways to increase the CPAP adherence. Lowering level of CPAP pressure is very effective for the patients with severe degree OSA [3]. This is because, in patients with severe OSA, more pressure is required compared with patients with mild to moderate degree. The high pressure of CPAP is a major cause for patients to suffer from various reasons and to reduce the CPAP adherence rate.
Case Report
This patient was a 41-year-old female who had been recognized snoring since several years ago. She had been diagnosed with impaired glucose tolerance and hypertension for the past two years. To manage the metabolic syndrome and obesity, she decided to visit sleep clinic for sleep study and being treated for snoring. Her body mass index was 46.02 kg/m2. Epworth sleepiness scale was 18.
Overnight polysomnography (PSG) (Nox A1, Nox Medical, Reykjavik, Iceland) was performed for 8 hours in hospital. Her sleep structure showed no sleep stage 3 and rapid eye movement (REM) sleep period and decreased efficiency of sleep (77%). Apnea hypopnea index (AHI) was 60.5/hr and Supine AHI and non-supine AHI were 75.9 and 59.0/hr, respectively. The minimum oxygen saturation was very low with 48%. Her cephalometric measurement revealed narrow space in superior posterior airway and great distance between the hyoid and the mandible. Superior airway space is narrow (5.72 mm). The distance between the hyoid and the mandible is significantly increased with 25.03 mm.
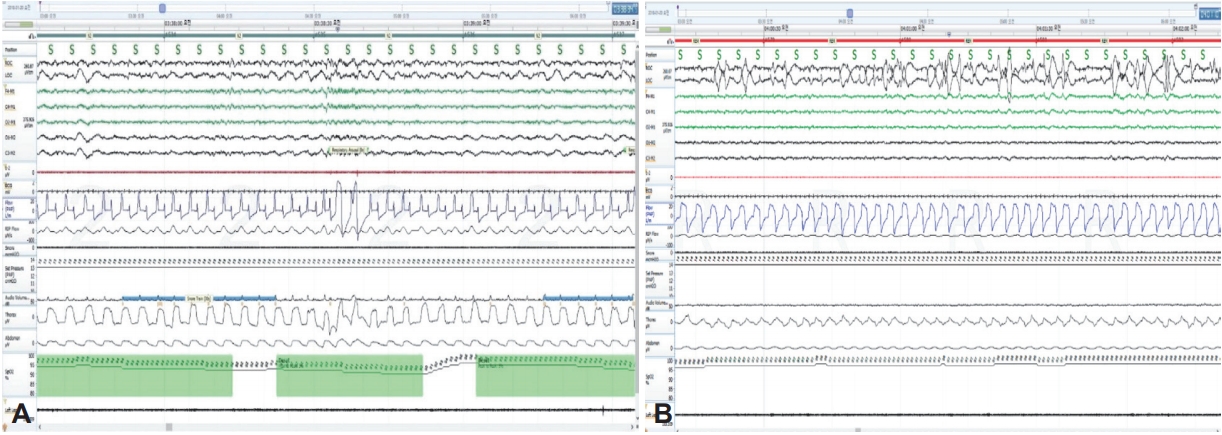
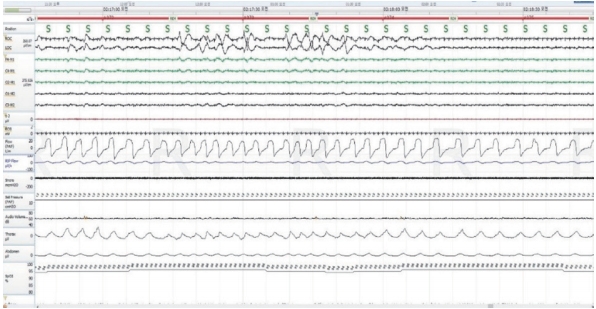
In order to have a period of adaptation and training prior to CPAP titration, adaptation period was used as the auto-setting CPAP (AirSense 10, ResMed Ltd, Bella Vista, Australia) at home. The average device pressure ≤90% of time for 2 weeks was reported to 14 cmH2O. She struggled with high pressure and complained about the discomfort of air leak forward to her eyes due to the large size of the nasal mask. She had CPAP treatment every night for one month, but the CPAP adherence for more than 4 hour was as low as 46%. We encouraged her to lose weight and regular exercise and she did exercise twice per week and restrict intake hard. However, she failed to weight loss. The average device pressure ≤90% of time have not been lowered. One month later, she underwent manual CPAP titration to make an optimal pressure. In addition, in order to reduce the pressure of CPAP, we proposed to vary the pillow height with CPAP titration. During manual CPAP titration, at the first step, the height of the pillow was 11.5 cm without lying on the pillow, and the height from floor to the backside of head was 4.5 cm with lying on the pillow. This pillow was at the same height as her usual pillow. At the first pillow trial during one and half hours, residual AHI was 4.3/hr and pressure of CPAP for eliminating apnea, hypopnea and loud snoring without arousal was 14 cmH2O (Fig. 1, Table 1). At the next step, the height of the pillow was 8 cm without lying on the pillow, and the height from floor to the backside of head was 2 cm with lying on the pillow. At the second pillow trial, residual AHI was 3.9/hr and the result of CPAP titration during next 2 hour including REM supine period was 13 cmH2O (Fig. 2, Table 1). The pressure of CPAP was reduced by only 1 cmH2O. We prescribed 13 cmH2O for fixed CPAP treatment with 8 cm low height pillow. She visited to the outpatient clinic two weeks later, and she said that she was more comfortable using CPAP with new prescribed pressure setting than before. She showed a better adaptation to the use of CPAP for 6 months (Table 1). She has still taken antihypertensive medication, but is better at controlling blood pressure and blood sugar level than before, and regularly exercising as prescribed.
Discussion
Head position is an important factor to reduce respiratory events in patients with OSA [4]. In patients with OSA, upper airway dimensions at all levels were significantly smaller than the healthy control [4]. Until now, lateral body position sleep is well known effective treatment option for reducing obstructive events during sleep in some patients with OSA. Recent study showed upper airway collapse is less severe during head rotation than in lateral head and trunk position [5]. In drug induced sleep endoscopic analysis in OSA, head rotation improved upper airway collapse in supine body position [6]. Based on several researches, the head position have been a significant factor for aggravating OSA and modifying factor for improving OSA as well as body position, recently. Some researchers have suggested that head position should be included in PSG recording along with body position [7].
Head position during night sleep is affected by the type and height of the pillow in use. A few studies have reported that pillows used for extension of the cervical spine helped snoring and apnea in patients with OSA [8,9]. However, the height and shape of the pillow are not clinically suggested for therapeutic purposes.
In severe OSA patients who required higher pressure of CPAP therapy than mild/moderate OSA patients, the effort to reduce the pressure slightly is important that directly affects the CPAP adherence. CPAP adherence was reported to be lower when the CPAP pressure was greater than 12 cmH2O which make more nasal problems [10]. Therefore, we should make additional concerns to increased CPAP adherence in patients with CPAP therapy using higher pressure over 12 cmH2O. It is necessary to consider the leak during CPAP treatment, the size and type of mask for patients’ comfortable use. And the device setting depending the various type of CPAP machine is also considered to increase adherence of CPAP therapy. Until now, head position and pillow effect are not major consideration in CPAP user with severe OSA as well as therapeutic effects on OSA. However, as mentioned above, these factors might play an important role in OSA patients as modifying the posterior airway space and prevent airway collapsing with extension of cervical spine. Based on this case, applying the pillow modification to all CPAP therapy is still week. It is needed to more researches for the effects of the height of pillow and head position for adherence of CPAP therapy.
In conclusion, height of pillow deserves consideration as a factor to promote CPAP adherence with lowering pressure, especially in the patient who are suffering with high pressure CPAP therapy.